If you work with women long enough—as I have—you start to notice a pattern. Most of us don’t think about bone health until we’re told we should. Often that’s far too late.
In reality, bone loss doesn’t suddenly begin at 65. It starts much earlier. Peak bone mass is typically reached in your late 20s to early 30s, and from then on, we’re either maintaining—or slowly losing—what we’ve built. By the time perimenopause arrives, the drop in oestrogen can accelerate bone resorption quite significantly.
The important part is this: we have far more influence over this process than most people realise
Protein and Bone Health: More Than Just Calcium
There’s a persistent tendency to reduce bone health down to calcium intake alone. Calcium matters, of course—but it’s only part of the picture.
Bone is a metabolically active tissue composed of a collagen matrix that becomes mineralised. That collagen structure is protein-dependent. Without adequate protein intake, you’re not just compromising muscle—you’re compromising the very scaffold that bone is built on.
From a clinical perspective, what we consistently see in the literature:
- Higher protein intake is associated with better bone mineral density, particularly in older adults
- Protein supports IGF-1 (insulin-like growth factor), which plays a role in bone formation
- Adequate protein reduces fall risk indirectly by preserving muscle mass and strength
In practice, when women under-eat protein—especially during busy midlife years—muscle loss (sarcopenia) begins quietly, and bone follows.
For most women I work with in their late 30s and 40s, a reasonable evidence-based target sits around 1.2–1.6 g of protein per kg body weight per day, particularly if they are training.

Muscle Is Not Optional Anymore
One of the biggest shifts that happens after 35 is that we can’t rely on “being active” in a general sense. Walking is excellent for health, but it’s not enough to maintain muscle or bone on its own.
Bone responds to load. Specifically, it responds to mechanical strain.
This is where resistance training becomes non-negotiable.
Research consistently shows that:
Programs that include progressive overload are the most effective.
Resistance and impact-based training improve or maintain bone mineral density.
Strength training enhances muscle mass, which in turn increases skeletal loading.
In real life, that translates to:
- Lifting weights (or using resistance bands) 2–3 times per week
- Including compound movements (squats, lunges, pushes, pulls)
- Gradually increasing load over time
You don’t need to train like an athlete—but you do need to challenge your system.
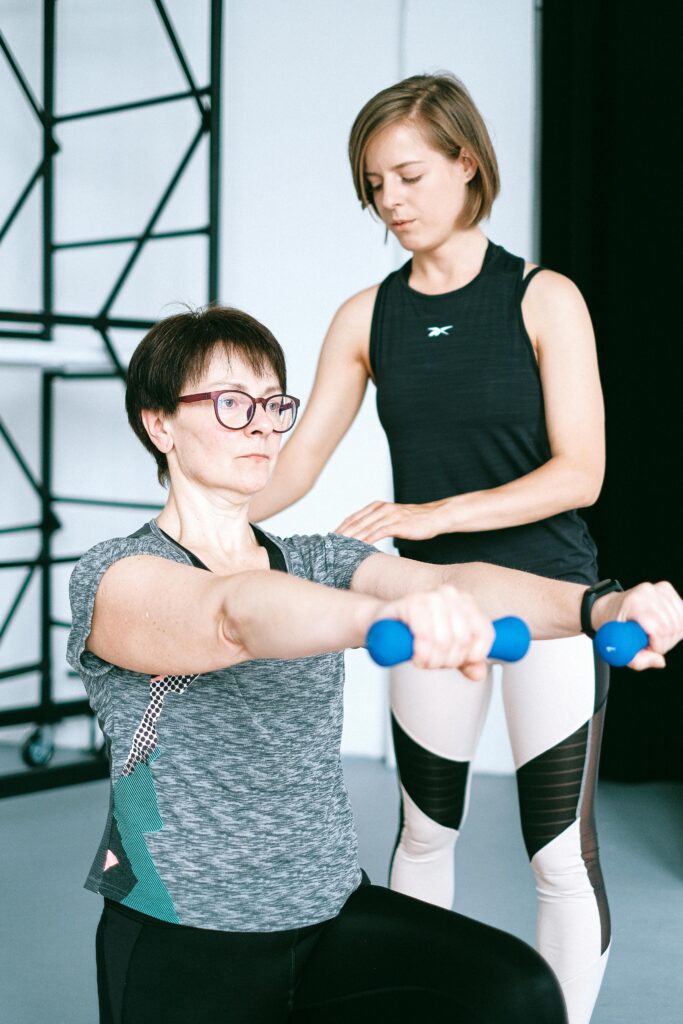
The Hormonal Context (That We Can’t Ignore)
Around the late 30s and into the 40s, oestrogen levels begin to fluctuate. Oestrogen has a protective effect on bone by reducing bone breakdown.
As levels decline:
- Bone turnover increases
- Bone resorption can outpace formation
- Loss of bone density accelerates
This is why the same lifestyle that “worked fine” in your early 30s may stop being sufficient.
Nutrition and training become less about optimalisation—and more about preservation.
Calcium and Vitamin D: Still Foundational
Even though protein and resistance training are often under-discussed, calcium and vitamin D remain essential.
In Ireland, vitamin D deserves particular attention. Between October and March, sunlight exposure is insufficient for adequate synthesis.
Evidence-based guidance typically suggests:
- Calcium: ~1000 mg/day (from food ideally)
- Vitamin D: 10–15 µg/day (400–600 IU), though higher supplemental doses are often recommended depending on status
Low vitamin D is associated with reduced calcium absorption and poorer bone health outcomes. It’s something I routinely check or recommend supplementing, especially in winter months.

Recovery, Energy Availability, and the Bigger Picture
One thing that often gets missed in conversations about bone health is energy availability.
Chronic under-eating—intentional or not—can negatively impact:
- Hormonal balance
- Bone turnover
- Recovery capacity
We see this clearly in conditions like RED-S (Relative Energy Deficiency in Sport), but milder versions are quite common in everyday life.
Add poor sleep into the mix, and you’re further impairing recovery, muscle maintenance, and hormonal regulation.
So while exercise and protein are key, they only work properly in a system that is:
- Adequately fuelled
- Well-rested
- Consistently supported
What This Looks Like in Practice
For most women over 35, a sustainable, evidence-informed approach would include:
- Resistance training 2–3 times per week
- Daily protein intake in the range of 1.2–1.6 g/kg
- Regular inclusion of calcium-rich foods (dairy, fortified alternatives, leafy greens)
- Vitamin D supplementation, particularly in Irish winters
- Prioritising sleep and recovery
- Avoiding chronic dieting or under-fuelling
A Final Thought
At 40, I can say this with both professional and personal clarity:
We have to stop treating bone health as something that belongs to our future selves.
By the time osteoporosis is diagnosed, the work is much harder.
What we do in our late 30s and 40s—how we train, how we eat, how we recover—quietly determines the resilience of our bones decades down the line.
This isn’t about aesthetics anymore. It’s about structure.

